Analysis of cerebrospinal fluid allows not only to confirm the diagnosis, but also to differentiate purulent and serous meningitis, identify the causative agent of the disease, determine the degree of intoxication, and also makes it possible to monitor the effectiveness of treatment.
To accurately and quickly diagnose meningitis, the Yusupov Hospital analyzes the patient’s cerebrospinal fluid. If no inflammatory processes are detected in the cerebrospinal fluid, then the diagnosis of meningitis is completely excluded.
Symptoms
Almost all patients have at least 2 of the typical four symptoms:
- Fever;
- Headache;
- Stiff neck;
- Impaired consciousness with a score of less than 14 points on the Glasgow scale.
A hemorrhagic rash is typical for meningococcal infection (rarely for pneumococcal, staphylococcal) and is localized on the torso, arms, legs, and butt. A rash on the face, and especially the earlobe and conjunctiva, is an unfavorable prognostic sign.
Diagnostics
Laboratory and instrumental studies:
- General urine analysis;
- Complete blood count with leukocyte formula;
- Biochemical studies: plasma glucose, blood urea and creatinine, blood electrolytes;
- Chest X-ray;
- HIV test;
- PCR – diagnostics;
- CT or MRI of the brain.
According to existing rules, a computed tomography (or MRI) scan of the brain should be performed before a lumbar puncture. These methods make it possible to exclude SAH, hematomas, abscesses and other space-occupying formations, as well as clarify the condition of the basal cisterns of the brain. Those. identify contraindications to lumbar puncture and clarify the diagnosis. But if CT or magnetic resonance imaging cannot be done within 1-2 hours from the moment the patient is admitted, then lumbar puncture should not be postponed until later.
CSF analysis
Analysis of cerebrospinal fluid (CSF) can confirm the diagnosis of meningitis.
| Table 1. The most typical changes in the cerebrospinal fluid in patients with meningitis | ||||
| Defined indicators | Normal values | Bacterial meningitis | Viral meningitis | Tuberculous meningitis |
| CSF pressure | 90-200 mm water. Art. | Often elevated | Normal or sometimes elevated | Often elevated |
| Number of cells | Lymphocytes, no more than 5 in 1 µl | Typically: 1000-10000 cells per 1 µl, neutrophilic leukocytes predominate | 20-200 cells in 1 µl, the content of lymphocytes is 60-90% of the total number of cells | 20-400 cells in 1 µl, the content of lymphocytes is 60-90% of the total number of cells |
| Pathogen | Not detected | Detected in 40-60% of cases | Not detected | Rarely detected |
| Protein concentration | 150-350 mg/l | above 1000 mg/l; | Within 1000 mg/l | above 1000 mg/l but there may be normal values |
| Glucose levels depend on blood glucose levels | 2.6-4.2 mmol/l. 55-60% of the concentration of glucose in the blood serum. | < 2 mmol/l; More precisely: less than 55-60% of the serum glucose concentration | > 2 mmol/l; More precisely: more than 55-60% of the glucose concentration in the blood serum | At the beginning of the disease it is not changed. After 1-2 weeks <2 mmol/l; More precisely: less than 55-60% of the serum glucose concentration |
| Lactate | 1.2-2.1 mmol/l | above 4.2 mmol/l | does not exceed 4.2 mmol/l. | varies |
Method of performing lumbar puncture
A lumbar puncture should be performed (preferably) before the person is given antibiotics. The puncture can be done in the intervertebral spaces L3-L4 (most often), L2-L3, L4-L5, and L5-S1. Doctors need to use 20 and 22 G needles. It is safer to perform the puncture when the patient is lying on his side. If it is not possible to obtain cerebrospinal fluid, the puncture is performed in a sitting position - higher cerebrospinal fluid pressure makes it easier to find anatomical landmarks for the puncture site.
Measurement of cerebrospinal fluid pressure should be carried out immediately after a successful puncture, and only after that the cerebrospinal fluid should be collected for laboratory tests. CSF pressure is measured with the patient lying on his side. Ideally, the cerebrospinal fluid should be collected in 4 sterile tubes:
– to determine the cellular composition of the cerebrospinal fluid;
– to determine microflora and its sensitivity to antibiotics;
– to determine the content of protein and glucose and other components;
– to determine the cellular composition of the cerebrospinal fluid (for comparison with the first tube).
To avoid diagnostic errors, laboratory tests should be carried out without delay.
Contraindications to lumbar puncture
- Lumbar puncture should not be performed if intracranial space-occupying formations (abscess, tumor, hematoma) are suspected.
- When signs of herniation appear - Cushing's syndrome (a combination of arterial hypertension and bradycardia), pathological pupillary reactions.
- Thrombocytopenia (platelet count <50×109/l).
- Coagulopathy, including those caused by taking medications.
- Inflammatory process in the puncture area.
If it was not possible to obtain cerebrospinal fluid (failure to do so, the patient’s refusal to undergo puncture, or contraindications to puncture), doctors should prescribe antibiotics to the patient. With bacterial meningitis, CSF pressure in most cases is higher than normal and there is a possibility of developing brain dislocation. Therefore, after a lumbar puncture, the person must be closely monitored (examination is carried out at least every 15-30 minutes during the first 4 hours).
If the neurological status after puncture progressively worsens, administration of osmotic agents (mannitol, sodium chloride 7.5%) should be started immediately. When to perform repeated lumbar punctures, the doctor decides individually. Some experts believe that in case of extremely severe meningitis, they should be performed every day. If the course of the disease is favorable, repeated lumbar punctures may not be performed.
Mumps meningitis
The causative agent of mumps meningitis belongs to the paramyxoviruses (family Paramyxoviridae, genus Paramyxovirus). The causative agent of mumps was first isolated and studied in 1934 by E. Goodpasture and K. Johnson. Virions are polymorphic, round virions have a diameter of 120-300 nm. The virus contains RNA and has hemagglutinating, neuraminidase and hemolytic activity. The virus agglutinates red blood cells of chickens, ducks, guinea pigs, dogs, etc. In laboratory conditions, the virus is cultivated on 7-8-day chicken embryos and cell cultures. Primary trypsinized cultures of kidney cells from guinea pigs, monkeys, Syrian hamsters, and chicken embryo fibroblasts are sensitive to the virus. Laboratory animals are insensitive to the mumps virus; only monkeys can reproduce a disease similar to human mumps. The virus is unstable, inactivated by heat, ultraviolet irradiation, contact with fat solvents, 2% formalin solution, 1% Lysol solution. The attenuated strain of the virus (L-3) is used as a live vaccine. The antigenic structure of the virus is stable. It contains antigens that can cause the formation of neutralizing and complement-fixing antibodies, as well as an allergen that can be used to perform an intradermal test.
The source of infection is only humans (patients with manifest and inapparent forms of mumps). The patient becomes infectious 1-2 days before the onset of clinical symptoms and in the first 5 days of illness. After the symptoms of the disease disappear, the patient is not contagious. The virus is transmitted by airborne droplets, although the possibility of transmission through contaminated objects (for example, toys) cannot be completely ruled out.
Susceptibility to infection is high. Children get sick more often. Males suffer from mumps 1.5 times more often than women. The incidence is characterized by pronounced seasonality (seasonality index 10). The maximum incidence occurs in March-April, the minimum in August-September. After 1-2 years, periodic increases in incidence are observed. It occurs in the form of sporadic diseases and epidemic outbreaks. In children's institutions, outbreaks last from 70 to 100 days, producing separate waves (4-5) with intervals between them equal to the incubation period. In 80-90% of the adult population, anti-mumps antibodies can be detected in the blood, which indicates the widespread distribution of this infection (in 25% of those infected, the infection proceeds inappropriately). After the introduction of immunization with live vaccine, the incidence of mumps decreased significantly.
Basic principles of management
They try to normalize body temperature, reduce headaches, and reduce the patient’s tension. For these purposes, non-narcotic analgesics, sedative therapy, and anti-nausea medications are used. Indications and implementation of artificial pulmonary ventilation follow the same principles as for patients with TBI.
In severe cases, due to impaired consciousness, vomiting, enteral food intake is often difficult. On the first day, less often, in the first 2 days, an infusion of saline solutions is used to replenish the loss of fluids and electrolytes. They try to make do with the minimum possible volumes - 1.5-2.5 liters per day. At the same time, hypotension must be corrected without delay. It is not recommended to use glucose solutions (if there is no hypoglycemia) derived from hydroxyethyl starch. For unstable hemodynamics, doctors use vasopressor infusions. It is better to give preference to norepinephrine (Norepinephrine) or phenylephrine (Mezaton).
Hyponatremia occurs in approximately 30% of patients with meningitis and can lead to increased cerebral edema. It must be eliminated immediately. As soon as the patient’s condition becomes stable, they switch to enteral feeding with nutritional mixtures. Any hyperglycemia that occurs should be promptly corrected. Seizures can dramatically increase intracranial pressure. In most patients with severe meningitis, the level of intracranial pressure is elevated.
With meningitis, an increase in ICP is often caused not so much by cerebral edema, but by excess production of cerebrospinal fluid. Therefore, lumbar punctures and furosemide injections are often effective when it comes to reducing ICP. If these actions fail to reduce ICP, cerebral herniation may occur; osmotherapy with mannitol or 3-7.5% sodium chloride solution should be used. In general, ICP quickly normalizes when antibacterial treatment is given. If the temperature drops, consciousness is clear, and focal neurological symptoms are not observed, then there is no need for decongestant therapy.
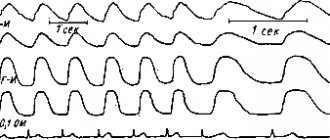
Clinical Chemistry: Cerebrospinal Fluid Analysis
Anyone who has watched the series about the brilliant Dr. House since school, remembers the scenes where the novice diagnostician Dr. Chase performs a lumbar puncture on the patient, and the latter lies on his side, writhing in pain, but nevertheless carries on a lively conversation with the doctor. Frankly, it must be admitted that not everyone of you, future graduates, will do this procedure, but being able to read the results of such tests is a necessary skill for every doctor. Most often, cerebrospinal fluid is sent for analysis to diagnose and monitor the development of inflammatory processes, neoplasms, and other damage to the central nervous system. An important element in diagnosing CNS diseases is anamnesis. Before starting the puncture, it is necessary to ensure that intracranial pressure is not increased. Normally, cerebrospinal fluid is clear and clean. Sometimes there may be cloudiness due to a large number of white blood cells. 100-300 cells per microliter of liquid causes a slight turbidity of the solution, 2000 - 10,000 already leads to the fact that the solution ceases to be transparent.
There is no need to panic if blood is detected in the cerebrospinal fluid. This is not necessarily a sign that the patient has subarachnoid hemorrhage or ventricular hemorrhage. Perhaps you hit a nearby vessel. In case of bleeding, the entire sample will be homogeneously red. If it gets into the vessel, as the needle moves, the sample will gradually become less and less transparent. To distinguish between old and new bleeding, the cerebrospinal fluid is centrifuged, causing fresh, intact red blood cells to settle at the bottom of the vessel. If the upper phase remains red, the sample is not examined further, since all the results will be false. Blood contains many more cells and proteins. Therefore, there is no point in analyzing even slightly scarlet samples. This fact often leads to disputes between laboratory staff and attending physicians. Doctors often ask to analyze the sample based on the calculation of 1000 red blood cells per 1 leukocyte. However, these results cannot be further studied due to partial hemolysis during sample removal - the risk of erroneous results is very high. Therefore, we recommend that everyone who will perform a lumbar puncture in the future do it correctly from the very beginning (this is better than coming to the patient again and admitting that they “injected incorrectly” and asking for another try). CSF that is pink, red-brown, or yellow in color may be a sign of xanthochromia (for example, as a result of the destruction of red blood cells already 2 hours after the start of bleeding), or it may indicate hyperbilirubinemia (bilirubin in high concentrations passes through the BBB). Xanthochromia as a result of the destruction of hemoglobin begins at least 3 days after bleeding. Using spectrometric tests, it is possible to determine the concentration of free hemoglobin, methemoglobin and bilirubin. During inflammatory reactions in the body, the concentration of fibrinogen in the cerebrospinal fluid (CSF) often increases. If the sample stands for more than 24 hours, the formation of a fibrin network can be observed. However, the diagnostic value of this phenomenon is minimal.
Let's talk first about the cells in the cerebrospinal fluid. The BBB consists of capillary endothelial cells and astrocyte processes (tight junctions). Inflammatory processes lead to disruption of the density of these contacts, which entails an increase in cells in the CSF. It is important to remember that the study should be carried out no more than an hour after the puncture, since the red blood cells disintegrate and their contents mix with the cerebrospinal fluid. Therefore, the sample should not even be stored in the refrigerator.
The number of cells in the cerebrospinal fluid is calculated using the same methods as in the case of blood (for example, using a Fuchs-Rosenthal chamber, or determining the number of leukocytes by diluting the sample with acetic acid). The Fuchs-Rosenthal chamber is capable of holding a volume of 3.2 microliters. Previously, results were written as a fraction divided by 2. For example, 5/3 cells. Now the number of cells is written based on the concentration per microliter (in this case, 2 cells per microliter of sample). Experienced laboratory technicians can distinguish between granulocytes and lymphocytes by counting them on a glass slide. The number of different cells is usually indicated as a percentage of the total number. To determine the number of leukocytes, special cytocentrifuges are used. Pappenheim staining of cells is extremely important for the diagnosis of tumor diseases. Devices for counting cells, of course, are also used, but in the cerebrospinal fluid you can find much fewer cells than necessary for them, so they often resort to manual counting.
Normal values per microliter of lumbar sample (for suboccipital or ventricular cerebrospinal fluid the values are lower): Newborns: leukocytes <15, erythrocytes <500. Adults: white blood cells <5, no red blood cells. Lymphocytes 60-80%, monocytes 40-15% of the total. A number of cells greater than five per microliter is called pleocytosis. The largest number of cells is found in bacterial meningitis (up to 20,000 per microliter), mainly granulocytes. With proper antibiotic therapy, the number of cells in the cerebrospinal fluid decreases sharply. With bacterial and viral meningitis, the number of leukocytes per milliliter of CSF can reach 1000. In the subacute proliferative stage of the disease, the number of leukocytes decreases, and the number of lymphocytes increases. During the remission phase, monocytes and lymphocytes can most often be seen in the cerebrospinal fluid. After brain surgery, an increase in all three types of cells is possible, which is a sign of aseptic inflammation. In the early phase of acute bacterial and viral meningitis, the number of leukocytes does not exceed 100 per microliter of sample. A poor prognostic sign at this point is a greater number of bacteria compared to an increase in the number of white blood cells. Tumor cells more often appear in the cerebrospinal fluid during various metastases. Primary tumor cells are detected only if the neoplasm itself is located close to the CSF.
As in the case of cells, disruption of the BBB permeability leads to an increase in the concentration of proteins in the CSF. In fact, to be more correct, we should talk not about permeability disorders, but about cerebrospinal fluid circulation disorders. It is the latter factor that causes its insufficient filtration in various diseases.
To determine the presence of albumin, special dye-coated strips are used, which are more sensitive to albumin than to globulins. The Biuret method, which was discussed in the previous post when we talked about proteins, is also used in diagnostics (before the test, the sample is treated with perchloric acid and trichloroacetic acid). Quantitative methods of analysis also include turbidimetric testing with trichloroacetic acid with protein precipitation or pyrogallol red molybdate.
Normal values (mg/l): Newborns : 430 – 1030 mg/l Children: 150-450 mg/l Adults: 200-400 mg/l Protein concentration reaches high values primarily with meningitis of bacterial etiology and can be 10 grams per liter of sample; it also increases in the acute phase of other inflammatory diseases of the meninges, with neuroimmunological pathologies, and with impaired microcirculation of the cerebrospinal fluid (hypolyquorhea or aliquorhea).
Brain cells produce three diagnostically significant proteins: NSE (neuron-specific enolase), S-100 (a dimer synthesized by astrocytes) and Tau protein (Microtubule-associated protein tau, MAPT). They enter the cerebrospinal fluid through the choroid plexus of the ventricles of the brain (plexus choroideus) or directly through the ependymal cells. Enolase (NSE) and S-100 increase during intracerebral bleeding and concussions and are important indicators for predicting the course of the disease. Tau and phospho-Tau proteins are found in Alzheimer's disease and Creutzfeldt-Jakob disease. The BBB functions according to almost the same laws as the filtration barrier in the kidney: the smaller the protein, the easier it passes through the barrier. Therefore, prealbumin (molecular weight 61 kiloDaltons) and albumin (66 kDa) still have a chance to overcome it, while immunoglobulin G (150 kDa) is much more difficult to do. It is worth recalling that albumin is synthesized exclusively by the liver, while immunoglobulins in inflammatory and tumor diseases can also be produced in the central nervous system.
It is clear that to compare the amount of protein in the cerebrospinal fluid we will also need a venous blood sample. That is why you should always remember that venous blood must be collected before puncture. If the patient is prescribed immunoglobulin or albumin infusion therapy, then the test results will also be overestimated.
It is worth noting that cerebrospinal fluid analysis is not the cheapest procedure. Such research requires special equipment. With its help, it is possible to determine the ratio of albumin and IgG, IgA or IgM in the cerebrospinal fluid in relation to plasma (Delpesh coefficient). Using isoelectric focusing and gel electrophoresis followed by staining with a solution containing silver ions, it is possible to determine individual subclasses of immunoglobulins depending on the number of kappa and lambda chains in them. In the same way, the presence of specific antibodies to viral antigens, for example, to the proteins of the herpes virus, rubella and measles, is determined.
You most likely will not have to master the above methods, unless after a series of these posts you fall in love with laboratory diagnostics. It is more likely that one day they will bring you a conclusion from a cerebrospinal fluid analysis, and it will look like a Reiber diagram. The diagram itself is based solely on empirical knowledge.
The coefficient under study strongly depends on the patient’s age, therefore, for each age group it is necessary to determine its own normal value. With pathologically increased protein synthesis in the central nervous system, the test result shows an increase in oligoclonal antibodies. Oligoclonal antibodies are not found in blood plasma; they should also be distinguished from monoclonal ones, found in myeloma and Waldenström's macroglobulinemia and distributed both in the cerebrospinal fluid and in the blood plasma. Oligoclonal antibodies occur in 24-40% of cases in CNS infections. They play a great role in the early diagnosis of multiple sclerosis. There is a tendency to spread the method of determining specific antibodies in the cerebrospinal fluid for the differential diagnosis of various neurological diseases.
Another important diagnostic parameter is the concentration of glucose and lactate in the CSF. Glucose freely passes into the brain through the BBB with the help of a special transport protein. A low concentration of glucose in the cerebrospinal fluid most often indicates that it contains bacteria that consume it to maintain their vital functions. Viruses don't do this. Tumor cells also have a special appetite for glucose. By metabolizing it, they form lactate in large quantities. These two parameters (the concentration of glucose and lactate in the cerebrospinal fluid) are used, among other things, to monitor the consequences of a stroke and in the diagnosis of bacterial and viral meningitis and meningoencephalitis. This test should be performed immediately after sample collection because lactate concentrations increase within the first 30 minutes after CSF collection.
In acute bacterial meningitis, glucose concentrations are reduced and lactate levels are particularly high. Together with clinical symptoms, these changes are reliable evidence of the diagnosis. During the acute phase of viral meningoencephalitis, both parameters remain unchanged. With antibacterial therapy, the concentration of glucose increases sharply, and lactate decreases.
The severity of stroke also correlates with the concentration of lactate in the blood - if it increases by more than 4 mmol per liter of CSF, we can rather speak of a poor prognosis for the course of the disease and a larger area affected by ischemia. During generalized epileptic seizures, lactate increases in a similar way.
Source
Klaus Dorner. Klinische Chemie und Hämatologie. 8th edition, Stuttgart, 2013
Personnel protection and patient isolation
To prevent airborne spread of infection, patients with meningococcal infection or meningitis of unknown etiology are isolated during the first 24 hours of antibiotic therapy. Infection of personnel can occur during tracheal intubation, CPR, and artificial ventilation. Standard precautions must be taken.
The need for prophylactic antibiotics should be considered for ICU staff if a patient is diagnosed with meningococcal meningitis. The likelihood of infection remains for 24 hours after antibiotics are prescribed. The chance of infection is higher among younger employees and people over 60 years old.
Use any of the following schemes:
1. Ciprofloxacin tablets, 500 mg twice a day. per day for 2 days;
2. Rifampicin tablets, 600 mg every 12 hours for 2 days.
Acute bacterial meningitis
Today, modern diagnostic and treatment methods are used, but the mortality rate for bacterial meningitis reaches approximately 20%. It should be remembered that only after 24 hours do changes in the cerebrospinal fluid become characteristic of purulent meningitis. Therefore, if meningitis is suspected, doctors immediately prescribe antibiotics to the person.
Pathogen identification
Identification of the type of pathogen and determination of its sensitivity to antibacterial agents, in most cases, occurs with a great delay - after 3-4 days. In cases where the ongoing antibacterial therapy gives the expected effect and the patient’s condition becomes better, after obtaining the results of sensitivity to antibiotics, as a rule, antibiotics are not changed. If a significant improvement in the patient’s condition has not occurred by the time the results of the bacteriological examination are obtained, the antibacterial drug that is most effective against the isolated pathogen is prescribed.
Comprehensive study of cerebrospinal fluid in bacterial purulent meningitis
Bacterial purulent meningitis (BPM) takes a leading place in the structure of neuroinfections. Despite significant advances in the treatment of HBM, mortality over the past 40 years has remained at a stable level of 6–24%, depending on the etiology of HBM and the quality of treatment [1–5]. Research conducted in 2008–2014 improved the quality of medical care for patients with HD due to, among other things, the development and implementation of new methods for studying cerebrospinal fluid (CSF): polymerase chain reaction (PCR), lactate level, D-fibrin dimer (D-dimer). DF), lactate dehydrogenase (LDH) and its isoforms, protein fractions, pH, pO2 and pCO2, study of indicators of local humoral and cellular immunity.
Materials and research methods
The CSF was studied in 1806 patients with HD of various etiologies; the comparison group consisted of 25 patients with serous viral meningitis and 10 patients with non-inflammatory lesions of the central nervous system (CNS). Spinal puncture was performed upon admission to the hospital (acute period of illness), on days 3–5 (complicated course) and on days 8–18 of treatment.
Research results
Bacteriological examination of the CSF, being the “gold standard” of diagnosis, provides the etiological decoding of meningitis in no more than 30–40% of cases [1, 4, 6], and immunological methods, in particular, the latex agglutination reaction (LAR), in 60 % of cases [7, 8]. The use of PCR makes it possible to decipher the etiology of meningitis in the late stages of the disease and against the background of ongoing antibacterial therapy, when the bacteriological method does not give a positive result and the amount of capsular polysaccharide antigens in the CSF is not sufficient for their detection by the X-ray method [8–10]. The use of PCR also helps to differentiate viral and bacterial meningitis in doubtful cases, determining the treatment strategy for the patient. The use of PCR increased the efficiency of decoding the etiology of meningitis by an average of 40% compared to the results of bacteriological and immunological studies (N. meningitidis, H. influenzae and Str. pneumoniae), and in combination with other methods of etiological diagnosis of meningitis, it allowed to increase the deciphering of meningitis from 46% up to 88%, and with early admission and no treatment in 100% (Table 1).
According to the results of various diagnostic methods over the past 7 years, significant changes in the structure of the brainstem have been identified. As before, the leading pathogens of BGM (64%) are meningococcus and pneumococcus, and there is a decrease in the number of patients with meningococcal meningitis by 1.25 times (50.1–41%). Hemophilic meningitis is registered in children under 5 years of age, and due to the use of vaccination, the number of patients decreased by 2.5 times (from 9.9% to 4.0%). Significant is the increase over the past 5 years in the role of staphylococcal meningitis to 22.3%. The incidence of pneumococcal meningitis remains at a consistently high level (23%). In some cases, the causative agents of BGM were Listeria, Klebsiella, various types of streptococci, gram-negative bacteria - no more than 9% (Fig. 1).
The disadvantage of etiological diagnosis is the length of time it takes to obtain the result (up to three days) and often a negative result if previously taken antibacterial drugs. Therefore, to carry out empirical antibacterial therapy, it is necessary to use express diagnostic methods that allow, within 2–3 hours, to differentiate BGM from viral meningitis and other diseases of the central nervous system, and to identify criteria for the severity of the disease. In domestic and foreign literature, there are works on the study of lactate levels in the CSF [11, 12], D-DP [12–15], changes in acute phase proteins [12, 16–18], lactate dehydrogenase (LDH) and its isoforms simultaneously in the CSF and blood [12, 19, 20], indicators of acid-base status and electrolytes in the blood and CSF [21, 22]. However, these reports are descriptive in nature, regardless of the etiology, severity, treatment, and prognosis of HBM. The lactate level in the CSF can be considered as an integral indicator of the metabolic activity of the pathogen, which is inversely correlated with glucose. CSF lactate does not depend on its level in the blood, unlike glucose, since it is formed directly in the subarachnoid space and is a product of the metabolism of bacteria and leukocytes [23, 24]. With HD of various etiologies, the lactate level increases to 5.5–25.0 mmol/l (average 11.6 ± 0.7 mmol/l, normal 1.1–2.2 mmol/l). With viral serous meningitis and non-inflammatory lesions of the central nervous system, this figure remains in the range of 0.9–3.9 mmol/l (1.9 ± 0.5 mmol/l). A lactate level above 4.0–4.5 mmol/L is a reliable criterion for HDM, which allows it to be used as a reliable differential diagnostic test. Parallel determination of CSF and blood lactate is essential, since bacterial meningitis always develops against the background of bacteremia or the presence of a purulent-septic focus. The level of blood lactate, especially in secondary HMG (pneumogenic, otogenic, rhinogenic, sepsis), was determined from 3.1 to 4.8 mmol/l (normal 1–2.1 mmol/l) in the acute period. Changes in the dynamics of CSF lactate levels make it possible to evaluate the effectiveness of treatment (Table 2).
With effective antibacterial therapy, after 2–3 days the lactate concentration decreases by 1.5–2.0 times or more; in the absence of effect or unfavorable outcome of the disease, there was no positive dynamics, which indicates that the pathogen retains biological activity in the subarachnoid space. Thus, CSF lactate can be used as a diagnostic, differential diagnostic and prognostic biochemical marker in HBM. We have established the presence of components of the hemostasis system and fibrinolytic activity in the CSF during meningitis. Of greatest interest is the determination of D-DP, which is the main product of fibrinolysis [13–15]. Normally, the level of D-DF in the CSF does not exceed 0.5 µg/ml (500 mg/ml). In the acute period of the disease (upon admission), its amount in the subarachnoid space increases and is above 1.0 µg/ml in 90% of those examined. During fibrinolysis of the inflammatory purulent exudate, on days 3–7 of treatment, the amount of D-DP in the CSF continued to increase by an average of 1.7 times (especially with pneumococcal etiology of meningitis) and varied in individual patients from 3 to 21 µg/ml (on average 13.5 ± 1.41 µg/ml), which was significantly higher (p < 0.005) than at admission. In viral meningitis and non-inflammatory diseases of the central nervous system, the level of D-DP did not exceed 3.0 µg/ml (1.05 ± 0.28 µg/ml) (Fig. 2).
The content of D-DP in the CSF also correlates with other indicators characterizing the severity of the inflammatory process in the subarachnoid space. The correlation coefficient with cytosis was 0.48, with protein content - 0.65, with glucose level - 0.65, with lactate level - 0.73. At the same time, there was no fibrinogen in the CSF of the examined patients, which indicates a high coagulation activity of the CSF, leading to the formation of fibrinous clots in the membranes and substance of the brain. Thus, D-DF can be used as a diagnostic marker of HD, and the dynamics of D-DF can be used to judge the effectiveness of the therapy and, in the absence of its reduction, to predict an unfavorable outcome of the disease. Indicators characterizing BGM are also changes in CSF acidity [21, 24, 25]. The CSF pH is normally slightly alkaline, corresponding to the blood plasma due to an increase in pCO2 to 50–60 mmHg. Art. (norm 45 mm Hg). With the development of HBM, the cerebrospinal fluid of 84.5% became more acidic (pH 7.0–7.3). There is also a decrease in pO2 in the CSF in more than 50% of patients to 40–45 mm Hg. Art. (norm 60 mm Hg), these indicators had a direct correlation with the severity of the patient’s condition (Table 3).
With effective therapy over time, by the 3rd day of treatment for BGM, the pH of the cerebrospinal fluid increases by an average of 0.2 and is 7.25–7.35, pO2 increases (more than 60 mm Hg), which indicates an improvement in blood flow in brain, and pCO2 decreases, which normalize in the complicated course of the disease by 5–8 days of treatment. Thus, the CSF pH level can serve as a diagnostic criterion for HD, an objective indicator of the severity of the disease, and a criterion for assessing the effectiveness of therapy. Almost all enzymes involved in metabolism in the brain are found in the CSF [12, 24–27]. However, due to the low content in the CSF, the determination of their activity is associated with a number of difficulties. Of the detected enzymes, LDH is of greater diagnostic value - the most sensitive indicator of brain hypoxia and lactatrachia. LDH activity in the CSF increases with various brain lesions (normal range is 5.0–40.0 U/l) [19, 20]. Moreover, the study of the isoenzyme spectrum of LDH is more informative than the general activity. In healthy people, LDH activity in the CSF is lower than in the blood serum, and the LDH4 and LDH5 isoenzymes are most often not detected at all. Thus, it has been established that the activity of LDH1–2 in the CSF has a positive correlation with the severity of traumatic brain injury [18]. Inflammatory changes in purulent meningitis are caused by an increase in the proportion of LDH4–5. A study of LDH isoforms (LDH1, LDH2, LDH3, LDH4, LDH5) in the CSF in the acute period and in the dynamics of the disease of HD of various etiologies and severity showed that with HD in the CSF there is an increase in the activity of LDH4 and LDH5 by 2.5 times in the acute period diseases. There was a significant increase in the fractions of LDH4 and LDH5 in the CSF in all BGM, and with meningococcal meningitis their level reached a maximum already on the 1st day, with pneumococcal meningitis - by the 3rd–5th day of illness (p < 0.05) and averaged for LDH4 - 17 ± 9.5% (in the comparison group - 8.8 ± 5.7%), LDH5 - 33.2 ± 12.4 (3.3 ± 2.1). With a fatal outcome of the disease, the increase in LDH fractions is more significant than with moderate-severe HD, which reflects the involvement of the brain substance in the process in the complicated course of HD (Fig. 3).
The dependence of LDH activity in the CSF on protein content and pH has been established [21, 23, 24]. In viral meningitis, in contrast to BHM, the activity of the LDH1 and LDH3 isoenzymes in the CSF increased, which correlated with the content of lymphocytes. Thus, the appearance of LDH4–5 in the CSF can serve as a diagnostic criterion for HD, and the normalization of these indicators indicates the effectiveness of the therapy. An increase in protein levels in the CSF during inflammatory processes is due to an increase in the permeability of the vascular walls [24, 28]. In this case, the ratio of albumin to globulins ranges from 2–3. Albumins and globulins in the CSF are an important indicator of the permeability of the blood-CSF barrier (HLB), and are also markers of acute inflammation (acute phase proteins), since their function in HBM is the recognition of foreign agents, the formation of an antigen-antibody complex with them and their neutralization [12, 28]. The CSF proteinogram is significantly more informative compared to the total protein value, since in some cases, with a normal content of total protein in the CSF, significant fractional changes are detected during electrophoresis [12, 24, 25]. Using electrophoresis, CSF proteins can be divided into albumins, α-1-globulins, α-2-globulins, β-globulins and γ-globulins; we conducted these studies depending on the severity of the patient’s condition in the acute period and the dynamics of treatment. In all groups of patients with HD in the acute period of the disease, an increase was noted? -1-globulins in the CSF, which is presented in table. 4.
A significant direct correlation was revealed between the same indicators: albumin (R = 0.59) and α-2-globulins (R = 0.53) in blood serum and CSF, which confirms the increased permeability of HLB in patients with breast cancer. It has been established that during purulent inflammatory processes in the CSF there is an increase in the content of α-1-, α-2- and γ-globulins, which characterizes an acute inflammatory process in the subarachnoid space, and the percentage of albumin decreases. Upon admission to the hospital (days 1–3 of illness), with BGM, α-1-globulins in the CSF increase by 1.8 times and α-2-globulins by 1.5 times, in contrast to viral meningitis, in the absence of such abnormalities in the blood, which indicates the possible production of specific acute phase proteins in the acute period of the disease directly in the choroid plexuses of the brain. From the 5th day, γ-globulins increased 2 times compared to the control group (p < 0.05). In the following days (days 3–8 of treatment), CSF γ-globulins increased by 1.7–2.1 times compared to the control group (p < 0.05) in all examined patients with HD. Thus, an increase in α-1- and α-2-globulins in the CSF may have a differential significance between meningitis of HBM and meningitis of viral etiology (serous) and is a marker of acute inflammation in HBM, as opposed to viral meningitis. The cerebrospinal fluid electrophoresis method makes it possible to evaluate the effectiveness of therapy and has clinical and prognostic significance when comparing protein fractions of CSF and blood serum in patients with HD. As for γ-globulins, they are of both plasma and brain origin [27, 28]. An increase in γ-globulins in the CSF is associated with increasing processes of local sanogenesis (IgA and IgM). Changes in the proteinogram are not strictly specific, and they are used for diagnosis, differential diagnosis and prognosis of the disease along with other routine and specific indicators. Immunological methods occupy a significant place in liquor studies [29, 30]. The immune system of the central nervous system functions autonomously and is a factor of sanogenesis in HD; there is no significant correlation (p > 0.05) for all parameters between immunity indicators in the blood and CSF. We have found that there are significant differences between the indicators of cellular and humoral immunity in the blood and CSF. In the CSF, there was a significant activation of immune parameters that was large and qualitatively different from the blood. Thus, IRI in the CSF was 3.0 ± 0.4, in the blood 1.9 ± 0.3 (p < 0.05), which was associated with an increase in CD4+ to 62.7 ± 5.4% (in the blood 45 .1 ± 4.8%, p < 0.05). This indicates a high phagocytic activity of CSF leukocytes. It should also be noted that in two patients with IRI in the CSF less than one, late sanitation of the cerebrospinal fluid was observed (19 and 27 for treatment). Long-term pleocytosis during clinical recovery is due to a local immunocellular reaction with the accumulation of T-helper cells and an increase in IRI to 4.5–5.0. Cytotoxic activity in the CSF was carried out mainly due to CD8+, and in the blood - NKT. At the same time, the B-cell system is activated and Ig of various classes accumulates in the CSF. Despite the fact that the content of Ig in the CSF was many times lower than in the blood, their concentration per 1 g of protein was significantly higher, which suggests that Ig is produced directly in the subarachnoid space. Ig levels in g% protein also varied significantly. The IgA content per gram of protein in the CSF was 0.150 g%, in the blood - 0.043 g% (p < 0.001), i.e. 3.5 times higher, IgM, respectively, 0.239 g% and 0.030 g/m (p < 0.001) , i.e. 7.6 times higher. It is difficult, especially in severe cases, to assess the effectiveness of antibacterial therapy in the early stages, especially in patients with severe HD, which often leads to unjustified replacement of the antibacterial drug. For example, with Hib meningitis, replacement was performed in 68%, but was justified in only 28%. It is not always possible to clinically evaluate the effectiveness of treatment, because with ineffective etiotropic therapy, mistakes are made when a temporary therapeutic effect is achieved through detoxification and dehydration therapy. With effective antibacterial therapy, the lack of positive dynamics or negative dynamics in the patient’s condition can be caused by the progression of the inflammatory process as a result of bacteriolysis under the influence of bactericidal drugs, intracranial complications (progression of cerebral edema-swelling, subdural and subarachnoid hematoma, blockage of the cerebrospinal fluid tract), extracranial complications ( pneumonia, etc.), activation of herpes infection, which is confirmed by the detection by PCR of replication of herpes viruses of types 1, 2, 5, 6, and febrile reactions to the administration of antimicrobial drugs. Our studies have shown that the effectiveness of etiotropic therapy in complicated disease can be assessed only on the basis of liquorological studies. They make it possible to evaluate the effectiveness of etiotropic therapy within 3 days in 91% of patients with meningococcal, in 82% with pneumococcal, in 88% with hemophilic influenzae and in 89% with meningitis of unknown etiology. It has been established that sometimes, with ineffective antibacterial therapy, the criteria for routine examination are not always informative; for example, there is a decrease in CSF pleocytosis by 1.5–2.0 times, and the percentage of neutrophils decreases. Therefore, the main criterion for assessing the effectiveness of antibacterial therapy is additional liquorological indicators: a decrease in protein levels by 2 times, an increase in glucose concentration by 1 mmol/l or more, a decrease in lactate and D-DP levels by 1.5–2.0 times within 2 –3 days, increase in pH by 0.2 and pO2 by 1.5 times, decrease in pCO2, decrease in LDH4 and 5 fractions, decrease in α-1- and α-2-globulins (Table 5).
The absence of positive dynamics or worsening of these indicators is prognostically unfavorable. Despite the existing criteria for discontinuation of antibiotics, in particular, a decrease in cytosis to 100 cells in 1 μl, in 5–10% of patients lymphocytic pleocytosis of up to 200–300 in 1 μl remains in the CSF for 1.0–1.5 months in good general condition . We have established that pleocytosis in these cases is caused by a local immunocellular reaction with the accumulation of T-helper cells and an increase in IRI to 4.5–5.0. At the same time, the B-cell system is activated and Ig of various classes accumulates in the CSF. Thus, the totality of this data in most cases allows, within 2–3 days, to realistically assess the effectiveness of treatment and make an informed decision on the duration of treatment with the same drug or on its replacement. Evaluation of the effectiveness of antibacterial therapy is objectively possible no earlier than after 2–3 days of treatment, and for pneumococcal meningitis - after 3–5 days.
Conclusion
The study of CSF allows one to obtain a huge amount of information about the nature of the pathological process in the membranes and substance of the brain, and in case of BGM it is the main method of diagnosis, differential diagnosis and assessment of the effectiveness of antibacterial therapy and prognosis of the disease. To increase the diagnostic value of CSF examination, it is advisable to determine the level of lactate, D-DP, and pH both in the acute period of the disease and during treatment.
Literature
- Lobzin Yu. V., Pilipenko V. V., Gromyko Yu. N. Meningitis and encephalitis. St. Petersburg: Foliot, 2006. 124 p.
- Koroleva M. A., Pokrovsky V. I., Mironov K. O. et al. Epidemiological monitoring of purulent bacterial meningitis in historical and modern aspects // Epidemiology and infectious diseases. Current issues. 2014. No. 2. P. 52–56.
- Vengerov Yu. Ya., Nagibina M. V. Practical aspects of diagnosis and treatment of bacterial purulent meningitis // Emergency Medicine. 2011. No. 3. pp. 23–28.
- Sorokina M. N., Ivanova V. V., Skripchenko N. V. Bacterial meningitis in children. M.: Medicine, 2003. 320 p.
- Bottomley MJ, Serruto D., Safadi MAP, Klugman KP Future challenges in the elimination of bacterial meningitis // Vaccine. 2012; 30 (Suppl. 2): B78–B86.
- Schuchat A., Robinson K., Wenger JD et al. Bacterial meningitis in the United States in 1995 // Active Surveillance Team. N.Engl. J. Med. 1997; 337(14):970–976.
- Bogomolov B.P. Diagnosis of secondary and primary meningitis // Epidemiology and infectious diseases. 2007. No. 6. pp. 44–49.
- Thigpen VC, Whitney CG, Messonnier NE et al. Bacterial meningitis in the United States, 1998–2007 // N. Engl. J. Med. 2011; 36 (21): 2016–2025.
- Vengerov Yu. Ya., Nagibina M. V. Diagnostic value of PCR for neuroinfections / Materials of the VIII scientific and practical conference “Infectious diseases and antimicrobial agents”. M., 2010. pp. 125–130.
- Tyutyunnik E. N. Use of PCR for diagnosing and predicting the course of meningitis. Author's abstract. Ph.D. M., 2001.
- Vengerov Yu.Ya., Nagibina M.V. et al. Clinical significance of lactic acidosis in purulent meningitis // Ter. archive. 2008. No. 80. pp. 33–35.
- Molotilova T. N. Comparative assessment of the biochemical characteristics of CSF and blood of patients with meningitis of various etiologies. Author's abstract. Ph.D. M., 2012.
- Papayan L. P., Knyazeva E. S. D-dimer in clinical practice. M., 2002.
- Gilmanov A. Zh. D-dimer. What? How? Who? For what purpose? // Clinical and laboratory consultation. 2009. No. 6.
- Adam SS, Key NS, Greenberg CS D-dimer antigen: current concepts and future prospects. // Blood. 2009. Vol. 113. No. 13. P. 2878–2887.
- Rosly I. M., Shulyak Yu. A. Practical biochemistry. M., 2004. 167 p.
- Minoranskaya N. S., Minoranskaya E. I. The importance of inflammatory markers for the differential diagnosis of various forms of acute ixodid tick-borne borreliosis // Modern problems of science and education. 2014. No. 1.
- Watson MA, Scott MG Clinical utility of biochemical analysis of cerebrospinal fluid // Clin. Chem. 1995. T. 41. R. 343–360.
- Paz JM et al. Evaluation of determination of lactate dehydrogenase isoenzyme I by chemica inhibition with perchiorate or with 1,6-hexanediol // Clin. Chem. 1990. Vol. 36. P. 355–358.
- Berestovskaya V. S. Methods for determining the activity of lactate dehydrogenase // Terra medica nova. Journal for doctors of all specialties. 2008. No. 1. 17 p.
- Mardanly S. G., Pervushin Yu. V., Ivanova V. N. Cerebrospinal fluid, laboratory research methods and their clinical diagnostic significance: a textbook for specialists in clinical laboratory diagnostics Elektrogorsk. JSC "EKOlab", 2011. 72 p.
- Chernyaeva T. E. Acid-base status, gas composition of blood and cerebrospinal fluid in patients with meningococcal infection. Author's abstract. Ph.D. M., 1973. 17 p.
- Tkachuk V. A. Clinical biochemistry. M.: Publishing house GEOTAR-Media, 2004. 515 p.
- Fridman A.P. Fundamentals of liquorology (the study of brain fluid). Ed. "Medicine", 1971. 647 p.
- Seehusen DA, Reeves MM, Fomin DA Cerebrospinal fluid analysis // Am Fam Physician. 2003. Vol. 68. P. 1103–1108.
- Guseinov T. Yu. Carbohydrate metabolism of the brain under hypoxia // Anesthesiology and Reanimatology. 1991. No. 3. P. 14–17.
- Pikalyuk V. S., Bessanova E. Yu., Tkach V. V. Liquor as a humoral environment of the body. Simferopol: IT "Arial", 2010. 192 p.
- Babich G.N. Markers of damage to the blood-brain barrier during neuroinfections // Neuroimmunology. 2003. T. 103. No. 1. P. 51–56.
- Balmasova I. P., Vengerov Yu. Ya., Razdobarina S. E., Nagibina M. V. Immunopathogenetic features of bacterial purulent meningitis // Infectious diseases and epidemiology. 2015. No. 3. pp. 15–18.
- Mazankova L.N., Nasr M.A., Guseva G.D. et al. Features of cytokine production during meningococcal infection in children // Children's infections. 2010. T. 9. No. 1. P. 17.
M. V. Nagibina*, 1, Candidate of Medical Sciences Yu. Ya. Vengerov*, Doctor of Medical Sciences, Professor D. V. Chernyshev** T. M. Kovalenko** T. N. Molotilova**, Candidate of Medical Sciences E P. Mikhalinova** S. E. Razdobarina** T. S. Svistunova**, Candidate of Medical Sciences E. V. Belikova** L. B. Baykova** T. Yu. Smirnova** A. P. Safonova ***
* GBOU VPO MGMSU im. A. I. Evdokimova Ministry of Health of the Russian Federation, ** GBUZ IKB No. 2 DZM, *** Federal Budgetary Institution Central Scientific Research Institute of Energy of Rospotrebnadzor of the Russian Federation, Moscow
1 Contact information