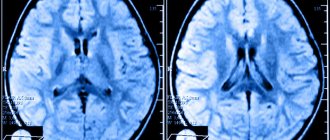
The term "hypoplasia" means "underdevelopment". Such defects of intrauterine development are also found in the arteries of the brain. In the arteries of the carotid artery basin, these anomalies exist in approximately 4% of people, and in the arteries of the vertebrobasilar basin - in every tenth person.
Despite the fact that the brain is the most energy-intensive organ and requires massive blood supply, hypoplasia of the arteries that supply it can go unnoticed for a long time. This is due to the characteristics of the cerebral circulatory system.
Most of the hemispheres receive blood from the system of internal carotid arteries, which form the anterior and middle cerebral arteries, as well as the anterior communicating artery. The posterior part of the hemispheres, the brainstem and the cerebellum are fed from the basin of two vertebral arteries, which merge in the cranial cavity into the main artery, from which the posterior cerebral and posterior communicating arteries are formed.
Due to the anterior and posterior communicating arteries, a connection is formed between the arterial basins of the brain, forming a circle. It is called Willis, and within its limits a compensatory flow of blood into areas with reduced arterial blood flow is possible, including due to hypoplasia of any segment of the artery. It is this feature of the brain’s blood circulation that ensures the long-term asymptomatic course of most hypoplasias, which often become an accidental discovery.
Clinical manifestations of hypoplasia of the cerebral arteries occur against the background of another pathology that worsens the conditions for compensation of cerebral circulation. Most often this is atherosclerosis of cerebral vessels or diseases of the cervical spine. As a result, transient ischemic attacks and ischemic strokes may occur.
What is hypoplasia? Causes, signs, treatment of hypoplasia
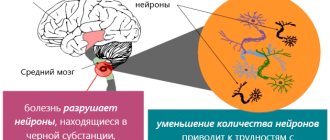
Hypoplasia is the underdevelopment of any organ or tissue - this is a common and main feature of pathology, be it hypoplasia of the kidneys, brain, or hypoplasia of a segment of the right or left vertebral artery.
In humans, underdevelopment of individual organs most often occurs. So, this pathology can affect the brain, but not the entire central nervous system, or one lung without involving the second and upper respiratory tract.
Pathology occurs due to a malfunction during intrauterine development. The most common causes of hypoplasia development:
- a failure that occurs during the initial formation of germ cells;
- incorrect intrauterine position of the fetus;
- scanty amount of amniotic fluid;
- bad habits of the expectant mother - smoking, drinking alcohol and drugs (most often they cause brain hypoplasia);
- infectious diseases of women during pregnancy;
- abdominal injuries of a pregnant woman;
- exposure to physical factors - elevated temperature, radiation;
- exposure to toxic compounds and harmful metabolic products.
Hypoplasia is not always detected on time. The success of diagnosis depends on the degree of underdevelopment and which organ is affected. Thus, to identify signs of tooth enamel hypoplasia in a child, an examination by an experienced dentist is often sufficient. While diagnosing renal underdevelopment will require additional instrumental examination methods.
Underdevelopment of the entire organism is called dwarfism.
Difficulties in diagnosing thrombosis of the cerebral veins and venous sinuses
Thrombosis of the cerebral veins and venous sinuses is more common in young women than in men, but is generally rare (up to 1% of all cases of cerebral infarction) [1]. According to ISCVT (International Study on Cerebral Vein and Dural Sinus Thrombosis, 2004), the incidence annually is 3–4 cases per 1 million in adults and up to 7 cases per 1 million in children. The mortality rate for this disease ranges from 5 to 30%; during more than 2 years of observation, a corresponding figure of 8.3% was recorded. At the same time, more than 90% of patients had a favorable prognosis. The main risk factors for the development of thrombosis of the cerebral veins and venous sinuses in the population are infectious inflammatory processes (otitis, mastoiditis, sinusitis, septic conditions) and non-infectious causes. Non-infectious causes of thrombosis of the cerebral veins and venous sinuses can be localized or general. The most commonly cited are traumatic brain injury, tumors, head and neck surgery, and pacemaker implantation or central venous catheter placement. Common conditions that contribute to thrombosis of the cerebral veins and venous sinuses include conditions such as hemodynamic compromise (eg, congestive heart failure, dehydration), blood disorders (polycythemia, sickle cell disease, thrombocytopenia), and coagulopathy (disseminated intravascular coagulation syndrome). , deficiency of antithrombin, protein C and protein S), as well as thrombophilic conditions associated with pregnancy, childbirth and the use of oral contraceptives, antiphospholipid syndrome, systemic vasculitis. However, in 15% of cases the cause of sinus thrombosis remains unknown [5]. Difficulties in diagnosing thrombosis of the cerebral veins and venous sinuses are due to the polymorphism of its clinical picture and the variability of the structure of the cerebral venous system. Anatomical features of the structure of
the cerebral venous system
In the development of thrombosis of the cerebral veins and sinuses, an important role is played by the anatomical features of the structure of the cerebral venous system (Fig. 1).
Unlike arteries and peripheral veins, cerebral veins lack a muscular wall and valve apparatus. The venous system of the brain is characterized by “branching”, a large number of anastomoses and the fact that one vein can receive blood from the basins of several arteries. Cerebral veins are divided into superficial and deep. Superficial veins - the superior cerebral vein, the superficial middle cerebral vein (Labbe vein), the inferior anastomatic vein (Trolar vein), the inferior cerebral veins - lie in the subarachnoid space and, anastomosing among themselves, form a network on the surfaces of the cerebral hemispheres. The main mass of venous blood from the cortex and white matter flows into the superficial veins, and then into the nearby sinus of the dura mater. Blood enters the deep cerebral veins from the veins of the choroid plexus of the lateral ventricles, basal ganglia, thalamus, midbrain, pons, medulla oblongata and cerebellum. The superficial and deep veins drain into the sinuses of the dura mater. The superficial veins drain mainly into the superior sagittal sinus. The main collectors of the deep veins are the great cerebral vein (vein of Galen) and the straight sinus. Blood from the superior sagittal and direct sinuses enters the transverse and sigmoid sinuses, which collect blood from the cranial cavity and drain it into the internal jugular vein. In the development of thrombosis of the cerebral veins and venous sinuses, 2 mechanisms are involved that determine the symptoms of the disease. The first is occlusion of the cerebral veins, causing cerebral edema and impaired venous circulation. The second link in the pathogenesis of thrombosis of the cerebral veins and venous sinuses is the development of intracranial hypertension due to occlusion of large venous sinuses. Normally, cerebrospinal fluid is transported from the cerebral ventricles through the subarachnoid space of the lower and superolateral surfaces of the cerebral hemispheres, adsorbed in the arachnoid plexuses and flows into the superior sagittal sinus. With thrombosis of the venous sinuses, venous pressure increases, as a result of which the absorption of cerebrospinal fluid is impaired and intracranial hypertension develops [5]. Both of these mechanisms determine the clinical symptoms of sinus thrombosis. Clinic and diagnosis
Clinical manifestations of thrombosis of the cerebral veins and venous sinuses depend on the location of thrombosis, the speed of its development and the nature of the underlying disease.
Severe disorders of the venous circulation are characterized by headache, vomiting, swelling of the optic discs, focal and generalized convulsions, and progressive depression of consciousness. However, with early recognition of the process, the clinical picture may be less pronounced. Focal neurological disorders can occur with isolated thrombosis of deep or superficial veins or with the spread of thrombosis from the sinuses to the veins. Meningeal syndrome is considered a rare manifestation of uncomplicated sinus thrombosis. Cerebrospinal fluid pressure, according to most authors, is normal or moderately elevated. The composition of the cerebrospinal fluid can be either unchanged or with a slightly increased protein content and pleocytosis of no more than 200/3 [1, 11–13]. Septic thrombosis of the transverse and sigmoid sinuses is characterized by a pronounced range of body temperature, leukocytosis, and accelerated ESR, but the use of antibiotics can smooth out these manifestations. Swelling of the mastoid area, pain on palpation, and less filling of the internal jugular vein on the affected side are very common. Sometimes thrombosis of the sigmoid sinus spreads to the internal jugular vein, which is accompanied by local inflammatory changes along the vein [1]. In contrast to arterial thrombosis and thromboembolism, neurological symptoms in thrombosis of the cerebral veins and venous sinuses more often develop subacutely - within a period of several days to 1 month. (50–80% of cases), although an acute onset may also occur (20–30% of cases) [6]. The most common symptom of thrombosis of the cerebral veins and venous sinuses is intense headache (92% of patients), which is a reflection of the development of intracranial hypertension. It resembles the pain of subarachnoid hemorrhage and is not relieved by analgesics. In addition, according to ISCVT et al. [1, 7–13], the following symptoms are identified: – motor disorders – 42%; – convulsive syndrome – 37% (including status epilepticus – 13%); – psychomotor agitation – 25%; – aphasia – 18%; – visual impairment – 13%; – depression of consciousness (stunning, stupor, coma) – 13%; – disorders of the innervation of cranial nerves – 12%; – sensitivity disorders – 11%; – meningeal syndrome – 5%; – vestibulo-cerebellar disorders – 1%. In the long-term period, the most common symptoms are headache (14%) and convulsions (11%). The cavernous and superior sagittal sinuses are relatively rare sites of infection. More often, the intracranial process is the result of the spread of infection from the middle ear, paranasal sinuses, skin near the upper lip, nose and eyes. With thrombophlebitis of the marginal sinus, which usually occurs against the background of inflammation of the middle ear or mastoiditis, pain in the ear and pain when pressing on the mastoid process appear. After a few days or weeks, fever, headache, nausea and vomiting appear due to increased intracranial pressure. Swelling in the mastoid area, dilation of the veins and pain along the internal jugular vein in the neck occur. When the internal jugular vein is involved in the pathological process, pain in the neck and limitation of its movements are observed. Drowsiness and coma often develop. In 50% of patients, swelling of the optic discs is detected (in some patients it is unilateral). Seizures occur, but focal neurological symptoms are rare. The spread of the pathological process to the inferior petrosal sinus is accompanied by dysfunction of the abducens nerve and trigeminal nerve (Gradenigo syndrome). Thrombophlebitis of the cavernous sinus is secondary to oculonasal infections. The clinical syndrome is manifested by swelling of the orbit and signs of dysfunction of the oculomotor and trochlear nerves, the orbital branch of the trigeminal nerve and the abducens nerve. Subsequent spread of infection to the opposite cavernous sinus is accompanied by the occurrence of bilateral symptoms. The disease can begin acutely, with the appearance of fever, headache, nausea and vomiting. Patients complain of pain in the eyeball area, pain in the orbital area when pressed. Chemosis, edema and cyanosis of the upper half of the face are noted. Consciousness can remain clear. Ophthalmoplegia, sensory disturbances in the area of innervation of the ophthalmic branch of the trigeminal nerve, retinal hemorrhages and papilledema may occur. Infection of the superior sagittal sinus can occur when the infection is transferred from the marginal and cavernous sinuses or spreads from the nasal cavity, the focus of osteomyelitis, the epidural and subdural areas. The disease is manifested by fever, headache, swelling of the optic discs. Characteristic is the development of convulsive attacks and hemiplegia, first on one side and then on the other due to the spread of the pathological process to the cerebral veins. Movement disorders may manifest as monoplegia or predominant involvement of the lower extremities. All types of thrombophlebitis, especially those caused by infection of the ear and paranasal sinuses, can be complicated by other forms of intracranial purulent processes, including bacterial meningitis and brain abscess. Due to the absence of pathognomonic clinical symptoms of the disease, instrumental and laboratory research methods are of utmost importance in diagnosing thrombosis of the cerebral veins and venous sinuses. In recent years, the improvement of neuroimaging technologies has opened up new opportunities for the diagnosis of sinus thrombosis (MRI, MR, CT venosinusography). For example, when performing MRI in standard modes, it is now possible to determine signs of venous thrombosis, expressed in increased signal intensity in the T1 and T2 modes, as well as T2-FLAIR from the altered sinus (Fig. 2). When performing MR venosinusography, a decrease in the signal from blood flow in the right transverse sinus is detected, as well as a compensatory increase in the signal from blood flow in the left transverse sinus (Fig. 3). If after an MRI or CT examination the diagnosis remains unclear, it is possible to perform contrast digital subtraction angiography, which can detect not only sinus thrombosis, but also the rare isolated thrombosis of the cerebral veins. Also, during this study, it is possible to identify dilated and tortuous veins, which is an indirect sign of thrombosis of the cerebral venous sinuses [14]. At the same time, a careful assessment of neuroimaging data is necessary to exclude errors in diagnosis, which may include, for example, hypoplasia or congenital absence of the sinus [6, 15]. Treatment
As already noted, the development of symptoms in thrombosis of the cerebral veins and venous sinuses is based on occlusion of the cerebral veins and sinuses, changes in brain tissue and the development of intracranial hypertension. This combination is potentially dangerous and may be associated with a poor prognosis in patients with thrombosis of the cerebral veins and venous sinuses. Therefore, it is necessary to carry out complex therapy, including pathogenetic therapy (recanalization of sinuses) and symptomatic therapy (fighting intracranial hypertension, infection) [1, 4, 10]. The main goal of therapy for thrombosis of the cerebral veins and venous sinuses is to restore their patency. Currently, the drugs of choice in this situation are anticoagulants, in particular low molecular weight heparins (LMWH). According to research, the use of direct anticoagulants in the acute period of thrombosis of the cerebral veins and venous sinuses improves the prognosis and reduces the risk of death and disability [16]. In addition, the ISCVT study obtained the following data for 80 patients with cerebral vein and venous sinus thrombosis treated with LMWH: 79% of them recovered, 8% remained mildly symptomatic, 5% had significant neurological impairment, 8% of patients died [1]. These data indicate the effectiveness and safety of the use of LMWH in the acute period of thrombosis of the cerebral veins and venous sinuses. In case of development of septic sinus thrombosis, antibacterial therapy should be carried out using high doses of broad-spectrum antibiotics, such as cephalosporins (ceftriaxone, 2 g/day IV), meropenem, ceftazidine (6 g/day IV), vancomycin ( 2 g/day i.v.). At the same time, there is no consensus on the feasibility and safety of anticoagulant therapy, although most authors adhere to the tactics of managing such patients with LMWH [18]. At the end of the acute period of thrombosis of the cerebral veins and venous sinuses, it is recommended to prescribe indirect oral anticoagulants (warfarin, acenocoumarol) at a dose at which the international normalized ratio (INR) is 2–3. Direct anticoagulants are administered to the patient until the INR reaches target values. In case of thrombosis of the cerebral veins and venous sinuses during pregnancy, the administration of indirect anticoagulants should be avoided due to their teratogenic potential and the possibility of penetration through the placental barrier. In such cases, continued treatment with indirect anticoagulants is recommended [18].
Currently, there are no studies clearly regulating the duration of use of oral anticoagulants. According to the recommendations of EFNS (2006), indirect anticoagulants should be used for 3 months. for secondary thrombosis of the cerebral veins and venous sinuses, which developed in the presence of a so-called transient risk factor, from 6 to 12 months. – in patients with idiopathic thrombosis and in the presence of “minor” thrombophilic conditions, such as deficiency of proteins C and S, heterozygous mutation of Leiden factor or mutations in the prothrombin gene (G20210A). Lifelong anticoagulant therapy is recommended for patients with recurrent venous sinus thrombosis, as well as for the diagnosis of congenital thrombophilic conditions (homozygous Leiden factor mutation, antithrombin deficiency) [17]. In addition to basic therapy, measures should be taken to prevent complications such as seizures and intracranial hypertension. These conditions require management according to general rules (prescription of anticonvulsants, elevated head of the bed, mechanical ventilation in hyperventilation mode with positive expiratory pressure, administration of osmotic diuretics). The effectiveness of glucocorticosteroids for cerebral edema resulting from thrombosis of the cerebral veins and venous sinuses has not been proven [19]. In some cases, in severe forms of thrombosis complicated by dislocation of brain structures, the issue of performing decompression hemicraniotomy, which is a life-saving operation, may be considered [20, 21]. This article presents the case histories of 3 patients who were at different times in the 2nd neurological department of the National Center of Neurology with a diagnosis of cerebral sinus thrombosis. The goal is to demonstrate modern capabilities for diagnosing and treating venous circulatory disorders. Patient K., 31 years old,
was admitted to the National Center of Neurology with complaints of intense headache, nausea, and vomiting.
History of illness:
within 2 weeks.
received treatment for herniated intervertebral discs using large doses of glucocorticosteroids and diuretics. On February 8, 2010, an intense headache that was not relieved by taking analgesics, nausea, vomiting, and photophobia suddenly appeared. The condition was regarded as increased intracranial pressure, and therefore diuretics were prescribed on an outpatient basis. On February 16, 2010, a generalized tonic epileptic seizure suddenly developed. The ambulance team hospitalized the patient to the clinic with a diagnosis of “Subarachnoid hemorrhage. Brain contusion,” which was subsequently removed. After treatment (venotonics, glucocorticosteroids, nootropics), the headache regressed. However, on March 7, 2010, headache, nausea, and vomiting suddenly reappeared. On March 19, 2010, the patient was hospitalized at the NCN. On examination:
pronounced expansion of the saphenous veins on the face.
The neurological status shows mild stiffness of the neck muscles. There are no focal symptoms. Laboratory research methods.
Lupus anticoagulant – 1.10%, negative result.
Antibodies to cardiolipins IgG – 15.8 U/ml, the result is weakly positive (normal is up to 10 U/ml). Homocysteine – 16 µmol/l (normal – up to 15 µmol/l). Antigen to von Willebrand factor – 273% (normal – up to 117%). Blood coagulation factors – without deviation from normal values. A blood test for thrombophilic mutations is negative. An examination by an ophthalmologist
revealed signs of intracranial hypertension: hyperemia and swelling of the optic discs, dilation and congestion of the veins in the fundus.
Instrumental research methods:
when performing MRI in T2 mode, an increase in the intensity of the MR signal from the superior sagittal and left sigmoid sinuses was noted (Fig. 4). When performing MR venosinusography, there is no blood flow in both transverse, superior sagittal and left sigmoid sinuses. Noteworthy is the increase in blood flow through the superficial cerebral and facial veins (Fig. 5). Diagnosis: thrombosis of both transverse, left sigmoid and superior sagittal sinuses. Treatment was carried out: nadroparin 0.6 ml 2 times/day subcutaneously for 10 days with a transition to warfarin (INR level 2–3), venotonics (diosmin orally, aminophylline intravenously), carbamazepine (convulsive syndrome). 10 days after the start of therapy, an improvement in well-being was noted - the headache decreased. During MR venosinusography, positive dynamics were noted - blood flow was restored in both transverse sinuses. After 4 months after treatment, the appearance of blood flow through the superior sagittal sinus was noted (Fig. 5). Anticoagulants are continued.
Patient M., 36 years old.
She was admitted to the National Center of Neurology with complaints of intense headache and pulsating noise on the right.
Life history:
migraine attacks without aura have been recurring since adolescence.
She took estrogen-containing contraceptives for a long time. Medical history:
On August 11, 2009, an intense headache suddenly developed, different in nature from ordinary migraine pain, which was not relieved by analgesics.
Later, a pulsating noise in the right ear, a feeling of “heaviness” in the head, nausea, staggering when walking, and weakness appeared. On August 21, 2009, she was hospitalized at the National Center of Neurology. Upon examination:
no cerebral, meningeal or focal symptoms were detected.
Laboratory research.
Lupus anticoagulant – 1.15%, negative result.
Antibodies to cardiolipins IgG – 30 U/ml (normal – up to 10 U/ml). After 3 months upon repeated examination at the Rheumatology Center - 10 U/ml, within normal limits. Homocysteine – 11 µmol/l (normal – up to 15 µmol/l). Coagulogram – without features. Blood coagulation factors – without pathology. A blood test for thrombophilic mutations is negative. Instrumental research methods.
Standard CT and MRI revealed no pathology. Contrast CT angiography revealed the absence of a signal from blood flow along the right sigmoid sinus (Fig. 6). Thrombosis of the right sigmoid sinus was diagnosed.
Treatment carried out:
nadroparin 0.6 ml 2 times/day subcutaneously with a transition to warfarin to achieve INR figures of 2–3 (6 months), aminophylline, rutoside. Due to repeated migraine attacks and prolonged pain syndrome, propranolol and antidepressants from the selective serotonin reuptake inhibition group were prescribed. During treatment, the headache disappeared. After 6 months During a control study (MR venosinusography), restoration of blood flow through the right sigmoid sinus was noted (Fig. 7). Taking into account the absence of signs of coagulopathy and a verified cause of sinus thrombosis, anticoagulant therapy continued for 6 months.
Patient K., 56 years old,
received on August 13, 2010. She made no complaints due to decreased criticism of her condition.
Life history:
arterial hypertension, deep vein thrombosis of the legs.
History of the disease:
On August 13, 2010, the color perception of surrounding objects suddenly became impaired (the color of the house changed).
Relatives noticed inappropriate behavior - the patient began to “talk.” Weakness developed in the left arm and leg, walking was impaired, and convulsive twitching appeared in the left arm and leg. The ambulance team transported her to the National Center. On examination:
partially disoriented in place and time.
Adynamic. Sleepy. Reduced criticism of one's condition. Speech is not impaired. Meningeal symptoms are negative. There are no oculomotor disorders. The face is symmetrical, the tongue is in the midline. There are no bulbar disorders. Mild left-sided hemiparesis with increased muscle tone of the plastic type. Tendon and periosteal reflexes are alive, S>D. Babinski reflex on the left. In the left limbs there are periodic clonic convulsive twitches of varying amplitude, lasting up to 1 minute. There are no sensory disorders. Laboratory tests:
homocysteine – 39 µmol/l (normal – up to 15 µmol/l), von Willebrand factor antigen – 231% (normal – up to 117%).
Lupus anticoagulant – 1.1%, negative result. Antibodies to cardiolipins IgG – 24 U/ml, the result is weakly positive (normal is up to 10 U/ml). Blood coagulation factors – without pathology. An examination by an ophthalmologist revealed signs of obstructed venous outflow. Instrumental studies:
MRI of the brain revealed an infarction with a hemorrhagic component, complicated by subarachnoid hemorrhage in the right hemisphere of the brain, as well as thrombosis of the right transverse sinus (Fig. 8).
Diagnosis
: infarction with a hemorrhagic component in the right hemisphere of the brain due to thrombosis of the right transverse and sigmoid sinuses, complicated by subarachnoid hemorrhage.
Treatment carried out:
enoxaparin 0.4 ml 2 times/day subcutaneously with switching to warfarin (continuous use) under the control of INR 2–3; venotonics (rutoside, aminophylline). Due to the detected hyperhomocysteinemia, folic acid and vitamin B12 were also prescribed. In addition, antihypertensive therapy was carried out. After 10 days from the start of therapy, the disappearance of clonic twitching in the left arm and leg, an increase in strength and range of motion were noted, the patient became more adequate, oriented in place and time. Upon repeated examination, the appearance of a signal from the blood flow along the right transverse sinus was noted (Fig. 9). Taking into account thrombosis of the right transverse sinus, a history of deep vein thrombosis of the legs, and an increase in homocysteine levels, the patient was recommended for continuous therapy with anticoagulants and folic acid.
Conclusion
In the 3 demonstrated cases, among the possible causes, the increased thrombogenic potential of the blood (increased level of antigen to von Willebrand factor, hormonal therapy, hyperhomocysteinemia) should apparently be put in first place. The thrombophilic state could serve as a trigger for the development of venous sinus thrombosis. Thus, in this situation, the main direction of pathogenetic therapy is the prescription of direct anticoagulants with a transition to indirect anticoagulants and maintaining INR values at 2–3. In addition, the importance of a thorough history taking has been demonstrated, in particular, close attention to the presence of an infectious process, traumatic brain injury, venous thrombosis, and taking medications that can provoke the development of a hypercoagulable state. The importance of a physical examination is also emphasized, which may reveal indirect signs of impaired venous outflow through the cerebral veins and venous sinuses (dilation of the facial veins in the first patient). In 2 patients, examination of the fundus revealed signs of impaired venous outflow and intracranial hypertension: congestive, swollen, hyperemic optic discs, dilated, congested veins in the fundus, absence of spontaneous venous pulse. All these signs, along with an indication of a new-onset, intense, difficult-to-treat headache, should give the clinician a reason to exclude disorders of cerebral venous circulation, which in turn is the key to successful treatment of patients and secondary prevention of this type of pathology.
Underdevelopment of the central nervous system. Brain hypoplasia
Intrauterine underdevelopment of the structures of the central nervous system is one of the most serious defects affecting the functioning of the entire organism.
You can guess about the underdevelopment of the central nervous system structures from the symptoms, which are detected almost from the moment of birth. Thus, with hypoplasia of the cerebellum, which is responsible for the coordination of movements, the child experiences incoordination and deterioration in muscle tone. And when he begins to walk, a balance disorder is revealed. Hypoplasia of the corpus callosum, which is responsible for the coordinated work of both hemispheres, can lead to a variety of consequences. First of all:
- muscle spasms;
- convulsions;
- impaired skin sensitivity and body temperature regulation;
- deterioration of auditory and visual memory.
Brain hypoplasia (or microcephaly) is a proportional underdevelopment of all its structures. In early childhood, such a disorder manifests itself as delayed growth and development, and in later childhood – serious intellectual impairment.
List of sources
- Shmidt E.V. Classification of vascular lesions of the brain and spinal cord // Journal. neuropathology and psychiatry named after. S.S. Korsakov. 1985. T. 85, No. 9. p. 1281-1288.
- Kurtusunov B. T. Variant anatomy of the vertebral arteries at the stages of human ontogenesis. Author's abstract. diss. Doctor of Medical Sciences Volgograd, 2011.
- Pizova N.V., Druzhinin D.S., Dmitriev A.N. Hypoplasia of the vertebral arteries and cerebrovascular accidents // Journal of Neurology and Psychiatry. 2010. No. 7. P. 56–58.
- Kometov A.V., Zhukova M.V. Variants of the structure of the vessels of the arterial circle of the cerebrum depending on the type of Kimmerle anomaly. Congress of Manual Therapists of Russia, 1st: Materials. M 1999; 32.
- Odinak M.M., Mikhailenko A.A., Ivanov Yu.S. and others. Vascular diseases of the brain. St. Petersburg: Hippocrates 1997.
Underdevelopment of the endocrine system organs
Hypoplasia of any organ of the endocrine system, as well as hypoplasia of the central nervous system structures, is of systemic importance, since many body functions depend on the hormones they produce. Thus, underdevelopment of the adrenal glands provokes disruptions in the production of steroid hormones, without which normal metabolism and immunity are impossible. Hypoplasia of the thyroid gland in women and men is fraught with metabolic disorders. And underdevelopment of the pancreas, which produces insulin, can cause diabetes.
Material and research methods
A study of patients with paroxysmal schizophrenia was conducted using MRI using the vascular mode. All patients underwent inpatient treatment at the Mental Health Clinic in 2009–2011. Clinical diagnosis of schizophrenia was carried out according to the criteria of the taxonomy of mental disorders adopted by the National Center for Mental Health of the Russian Academy of Medical Sciences and according to ICD-10. Of the 62 patients examined, 30 (1st group) had an attack-like-progressive (fur-like) form of the disease (F20.01, F20.02) with a stable or increasing defect and the persistence of residual hallucinatory-delusional disorders in remission.
In 32 patients (group 2), a recurrent (F20.03) form with remissions without residual psychotic symptoms and deficit disorders was identified. The age of the patients varied from 18 to 58 years, with the majority of patients aged from 18 to 39 years (57 people). The average duration of the disease from the moment of its manifest manifestations in most cases (47) did not exceed 9 years and in the 1st and 2nd groups of patients was 8.9 years and 4.9 years, respectively. 18 patients were admitted to a psychiatric hospital for the first time and practically did not take psychotropic drugs. 33 people took psychotropic drugs irregularly during interictal periods, and refused to take them before admission to the hospital. Syndromic psychopathological assessment of the condition of patients of groups 1 and 2 at the time of examination is reflected in Table. 1. None of the studied patients had severe somatic diseases, organic diseases of the central nervous system, or alcohol and drug addiction.
Table 1. Characteristics of the examined sample of patients with schizophrenia.
| Forms of schizophrenia | fur-like | recurrent | Total | ||
| Number of patients examined | 30 | 32 | 62 | ||
| Gender distribution | m | 15 | 14 | 29 | |
| and | 15 | 18 | 33 | ||
| Age range at the time of examination | 18-58 | 18-51 | 18 — 58 | ||
| Average age at the time of examination | 31,5 ± 9 | 29,6 ± 8,85 | 30,5 ± 9,3 | ||
| Average duration of illness | 8,9 | 4,9 ± 5 | 7 ± 7,7 | ||
| Leading syndrome | Catatonic-paranoid | 8 | 2 | 10 | |
| Hallucinatory-delusional | 15 | 3 | 18 | ||
| Affectively delusional | 7 | 26 | 33 | ||
The severity of the condition in the studied groups of patients with schizophrenia practically did not differ. In both forms, patients were hospitalized due to a rapid increase in psychotic symptoms, reaching a similar degree of severity (the average value on the Brief Psychiatric Scale BPRS for the paroxysmal-progressive form was 40.5 ± 6.8 points, and for the recurrent form – 40.7 ± 6, 3 points). Intergroup differences were noted only in the syndromic structure of psychosis: in the paroxysmal-progressive form, catatonic-paranoid and hallucinatory disorders had a greater share than in the recurrent form, with similar severity of affective disorders (Table 1).
The MRI examination was carried out on a 1.5T tomograph from Siemens (Germany) using the vascular mode without contrast. The tomograms were evaluated by an experienced neuroradiologist. The frequency of abnormalities in the condition of the cerebral ventricles (lateral, 3rd), subarachnoid spaces, fissures, as well as the condition of perivascular spaces, venous sinuses, including sigmoid and transverse sinuses, disorders of venous circulation in general, and anomalies in the structure of arteries was calculated. The significance of intergroup differences was calculated by Fisher's angular transformation. The intergroup difference was considered significant when the calculated Phi value was more than 1.64.
Underdevelopment of the genitourinary system
Underdevelopment of the genitourinary system manifests itself in the form of:
- kidney hypoplasia (possible underdevelopment of one kidney and absence of the second);
- underdevelopment of the testicles in men and the uterus in women, manifested by reproductive dysfunction.
During intrauterine development, a combination of both disorders is possible - from the urinary tract and the reproductive system.
In men, testicular hypoplasia can be accompanied by a reduction in the penis and scrotum. And in women with uterine hypoplasia, the ovaries, fallopian tubes and external genitalia (clitoris, labia) may not undergo such changes.
A woman’s reproductive function depends on the degree of endometrial hypoplasia of the uterus - if the inner layer of the uterus is underdeveloped, a fertilized egg will not be able to attach to the inner surface of this organ.
Introduction
Using intravital brain imaging methods, numerous data have been accumulated on anomalies of a number of cerebral structures in schizophrenia (cerebral ventricles, frontal and temporal cortex, thalamus, etc.) [2, 4, 16, 17, 20]. At the same time, the question of the nature of the detected changes remains not entirely clear and continues to be widely discussed in terms of the concepts of schizophrenia as a disorder of brain development, or an ongoing neurodegenerative process, relationships with hereditary and environmental factors [4, 5, 13, 14, 15, 18, 19].
Treatment of hypoplasia: general principles
There is no pathognomonic treatment (directed against provoking factors and slowing down the development of the disease) - medicine is taking the first steps in curing fetal diseases during intrauterine development. Rather, it is necessary to take preventive measures (in particular during pregnancy), which will help prevent failure in the formation of organs and systems, leading to disruption of tissue formation.
In the treatment of hypoplasia after the birth of a child and in adulthood, replacement therapy is practiced. So, with hypoplasia of the thyroid gland, accompanied by its hypofunction, the patient is injected with gland hormones.
You can read more about the tactics and methods of treating hypoplasia on our clinic’s website https://dobrobut.com.
Related services: Ultrasound examination Consultation with an obstetrician-gynecologist during pregnancy
Forecast
The prognosis is determined by many factors, in particular, unilateral/bilateral VA pathology, since with unilateral VA hypoplasia, blood flow compensation mechanisms develop, the functional state of the arterial-venous system of the brain, and the condition of the vascular wall (in particular, the presence of atherosclerotic plaques). After surgical treatment and drug rehabilitation, in most cases the lumen of the vertebral arteries can be normalized, and neurological symptoms regress.
Classification of the disease
Vascular disease affects and damages all areas of the brain. They provoke slow tissue development. The pathology may be congenital or appear with age.
Hypoplasia of the cervical artery most often begins to develop in the fetus in the womb.
The circle of Willis ensures normal blood supply to the brain. It is formed by large aortas of the spine with two branches. Usually the vessels develop evenly. A branched artery is responsible for natural blood supply. Vascular hypoplasia can be left-sided, right-sided or bilateral.
Hypoplasia of neck vessels disrupts blood supply and prevents normal nutrition of brain cells.
If you do not undergo diagnosis in time, cardiovascular failure and serious malfunction of the vestibular apparatus may develop.
First, you should undergo certain therapy, due to which the blood flow will return to normal.
Right artery lesion
The vertebral blood vessels first merge into a single basilar artery, which then divides into the right and left posterior cerebral artery. The right and left posterior communicating arteries depart from them, respectively. Through these blood vessels, blood flows to the posterior part of the brain, the cerebellum and the thalamic region.
Therefore, with hypoplasia of the right vertebral artery, a person’s motor activity, vision and psycho-emotional state are primarily affected. Some signs of pathology can be confused with manifestations of depression: decreased self-esteem, feelings of guilt, pessimism, sleep disorders, weather dependence, apathy and lethargy.
Sometimes the symptoms of hypoplasia are similar to the manifestations of tumor development:
- Frequent dizziness;
- Movement coordination disorder;
- Headache.
The main danger of the pathology is that hypoplasia leads to insufficient blood circulation in the vertebrobasilar region and the appearance of blood clots in it - thrombi. Degenerative changes in the substance of the brain may also appear and underlying diseases may develop, such as atherosclerosis, in which cholesterol plaques adhering to the walls will further reduce the lumen of the vessel and interfere with normal blood circulation.
Is it worth carrying out the silvering procedure?
Some dental clinics eliminate the initial stages of hypoplasia using the silvering method. The essence of this therapy is that a layer of active metals is applied to the teeth. Upon contact with enamel, crystals of silver phosphate and potassium fluoride are formed, protecting the enamel from destruction.
The Nutcracker Clinic does not use silver plating. We abandoned this method for several reasons:
- Poor efficiency. To remove plaque and restore the nervous structure of the incisors, you need to carry out about 5 procedures over six months.
- The drugs used often cause allergic reactions.
- In case of advanced caries, the procedure is contraindicated.
- After silvering, the enamel darkens, which causes psychological discomfort in the child.
Symptoms
Signs of hypoplasia are observed in older age, such as migraines, high blood pressure, drowsiness, psychological disorders and decreased sensitivity. The blood supply gradually returns to normal on its own. In such cases, the patient consults a doctor.
Possible symptoms:
- dizziness and pain;
- nerve dysfunction;
- disturbances of sensitivity, speech and motor apparatus;
- hallucinations.